Here you’ll find a range of information to help you feel in control of your sexual health and wellbeing. Whether you’re exploring your HIV prevention options, interested in long-acting contraception, or want support with your drug and alcohol use, you’ll find guidance and resources below. We also offer workshops and training to staff, community groups and influencers covering everything from HIV awareness and prevention through to cultural competency and LGBTQ+ inclusion.
If you have any specific questions, please do get in touch with our Testing and Prevention Team via:
Email: prevention@positiveeast.org.uk
Phone: 020 7791 2855 (option 3)
Chat with Pat, our sexual health chatbot (24 hours a day) by clicking HERE
Sexual Health Topics
PrEP
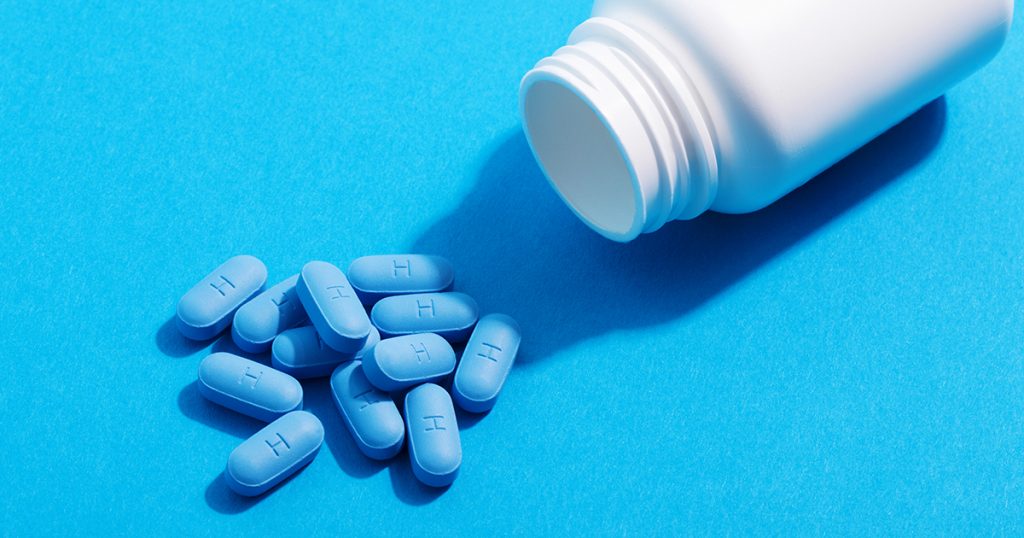
PrEP (Pre-exposure prophylaxis) is medication taken by HIV-negative people before and after sex to reduce the risk of getting HIV. PrEP only protects you from HIV and does not protect you from any other STIs.
PrEP was recently made available on the NHS through local sexual health (GUM) clinics. You can find a list of clinics offering PrEP in England here. Positive East can also support you with accessing PrEP, by contacting clinics on your behalf.
Before starting PrEP you will need to:
- Test for HIV to ensure you are HIV negative
- Have a kidney function blood test – note that the PrEP available on the NHS is not suitable for those with kidney function issues
These tests may be repeated after you have been taking PrEP for 6 weeks.
There are different ways to take PrEP depending on the sex you are having and how regularly you are having unprotected sex:
- Some people take one pill PrEP daily.
- If you’re having receptive vaginal sex, you’ll need to take one pill every day, 7 days before, and 7 days after sex.
- For anal sex you might try the T’s and S’s method which is is when someone takes PrEP on Tuesday, Thursday, Saturday and Sunday
- For anal sex you can also take ‘event-based’ PrEP – take 2 pills between 2 to 24 hours before sex, 1 pill 24 hours after the first double dose then a final pill 48 hours after that first double dose.
PEP
PEP (post-exposure prophylaxis) is a course of medication taken by HIV negative people after sex to reduce the risk of getting HIV. PEP needs to be taken within 72 hours of the potential risk. PEP is most effective when taken within 24 hours of the risk. It is medication that needs to be taken for 28 days.
PEP is available at sexual health (GUM) clinics or A&E. Find your sexual health clinic here.
PEP is free on the NHS but is not given routinely to everyone who asks for it. Only people who meet the guidelines will be offered PEP. You can find out more about the guidelines here.
U=U
HIV treatment and medication has improved vastly since the 80s when HIV was first discovered. There is still no cure for HIV, but we know all the tools and resources to ensure that people living with HIV in the UK have healthy and fulfilling lives in the same way that HIV negative people can. HIV medication reduces the number of copies of HIV in the someone’s system and for the majority people they can get this to levels known as ‘undetectable’. This does not mean they are no longer living with HIV but the amount of HIV in their blood is so low, it can not be picked in particular tests.
Studies have also shown that if someone has an undetectable HIV status, they are unable to pass on HIV to someone else when not using condoms. People who are undetectable can have children who are HIV negative and have unprotected sex without transmitting HIV. This is known as U=U or undetectable = untransmittable.
The U=U message is a very important message for anyone affected by HIV to address the fears and stigma of becoming HIV positive or knowing someone who is living with HIV.

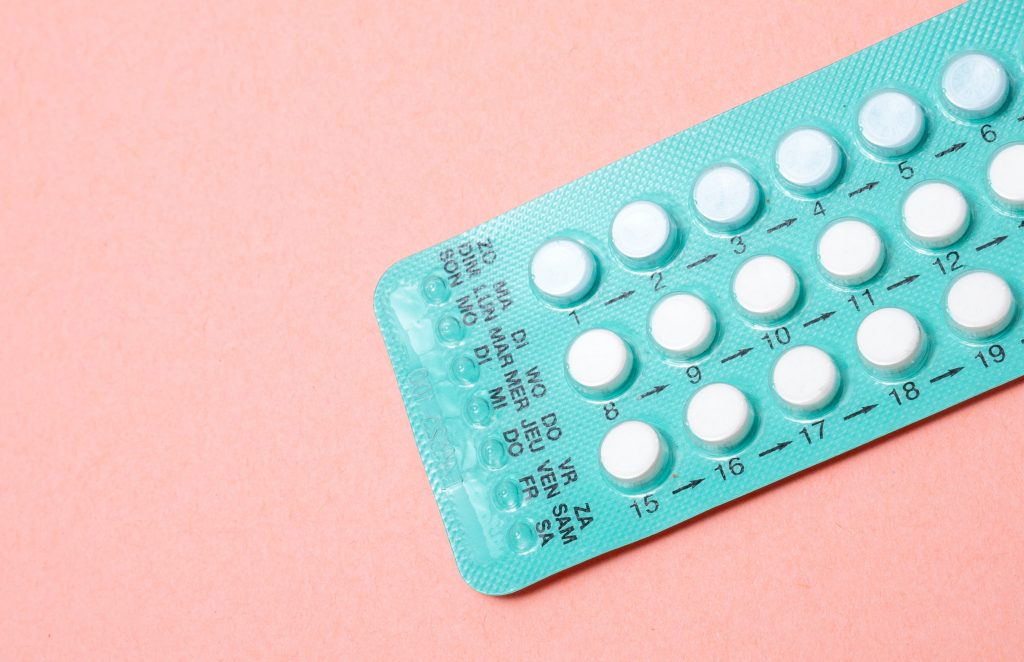
Contraception
The purpose of contraception is to prevent pregnancy. There are two main types of contraception: Hormonal and Non-hormonal
Hormonal contraception includes the contraceptive pill, the combined vaginal ring, the contraceptive patch, the progestogen only pill, the progestogen-only injection, the progestogen only implant and progestogen only intrauterine system (IUS).
These methods are called hormonal because they work by releasing hormones into the body which then prevent pregnancy. The hormones work by stopping ovulation, making cervical mucous thicker to stop sperm meeting an egg and by thinning the womb lining so eggs can not implant.
Some hormonal contraception may have side effects including breast tenderness, headaches and nausea. These often subside as your body gets used to the contraceptive.
Non-hormonal contraception is contraceptives that do not have any hormones in them. An IUD is a small copper and plastic device that is inserted into the womb. It works by creating an environment where sperm can not survive which then means the sperm can not reach the egg and fertilize it.
Diapapragms fit inside the vagina and cover the service and stop sperm entering the womb. The diaphragms need to be used with spermicide which contains chemicals to stop sperm meeting the egg.
External condoms are a made of very thin plastic or rubber. They are placed over an erect penis (and can also be used on sex toys and fingers to prevent STIs) and creates a barrier between sperm and the vagina. Condoms are beneficial because they do not only prevent pregnancy, but they are good at preventing STIs (sexually transmitted infections).
Internal condoms are similar to external but the interal condom goes inside the vagina and works by stopping sperm entering the vagina. They also give protection from STIs.
Emergency contraception is for people who have had unprotected sex recently and are worried about the risk of pregnancy. The pill also known as the morning after pill can be taken up to 72 hours after unprotected sex. The sooner it is taken the better.
It can be prescribed at GPs, sexual health clinics or A&E. It can also be prescribed at some pharmacies. Find a list of places that offer emergency contraception here.
A copper IUD can also be used as emergency contraception. This is the most effective option and can be used up to 5 days after unprotected sex.
Condoms & Lube
Condoms are the best form of protection from sexually transmitted infections (STIs). Condoms come in a range of sizes, textures, materials and flavours. It is important that you’re able to find the right fit and feel for you and your partner(s). Exploring what feels right for you and your partner(s) should be fun and enjoyable.
Before using a condom make sure it has a CE mark and that it has not passed its expiry date. If you are using sex toys do not forget to cover them with a condom and wash the toys after each use. If the condom comes off, open a new condom and put it on before continuing sex. Change condoms between partners and regularly replace them during longer sex sessions.
Lube makes sex smoother, more pleasurable and reduces the chance of a condom breaking. When using lube, stick to a silicone or water-based lube. Silicone-based lube will not damage condoms but may damage silicone sex toys. Avoid oil-based lubes like Vaseline, baby oil and lotions. They damage latex condoms.


Chemsex
The term chemsex addresses the availability of sex and drugs on hook-up apps amongst gay, bi and other men who have sex with men. Some people may feel that they need to have drugs in order to have different types of sex. The most common drugs used during Chemsex are:
- G, also known as GHB/GBL
- Meph, also known as meow meow
- Crystal meth
Some people may experiment with these drugs at hook-up parties and may find that it makes them feel more confident and helps them lose their inhibitions. In turn it can lead to some people finding themselves depending on these drugs in order to have sex. If these drugs aren’t taken correctly they can damage to the immune and nervous systems and at worst, prove fatal.
There’s several initiatives that can support in harm reduction include the Gay Men’s Health Collective’s PIP PACs which can contain colour-coded needles, a measuring spoon, condoms, lube and hydration sachets. It’s important that you pace yourself with both drugs and sex, that you outline your boundaries and safe words with partners beforehand, and that you only take drugs that you have sourced and administer yourself.
If you’re worried about the impact chemsex is having on you or someone you know, there is support from the following organisations:
- 56 Dean Street: https://dean.st/chems/
- https://www.letstalkaboutit.nhs.uk/other-services/chemsex-support/
- London Friend: https://londonfriend.org.uk/chemsex-support/
Helpful Resources
www.i-base.info – HIV treatment and prevention information
www.nat.org.uk – Myths and FAQs
www.tht.org.uk – all about HIV